Bruxism Explained: Causes, Signs and When to Speak to a Clinician
Waking with a tight, aching jaw or a dull morning headache can be easy to brush off – until it becomes a pattern. For many adults, these subtle signs point to bruxism, a condition involving unconscious teeth grinding or jaw clenching, often during sleep. Sometimes it’s a partner who notices the grinding first; other times, it’s a dentist flagging unexpected tooth wear. Either way, it can raise questions about causes, long-term effects, and whether exploring bruxism treatment is appropriate.
While bruxism is common, it’s often under-recognised and misunderstood. Understanding what’s behind the habit is an important first step before making any decisions about care. If you’ve been researching options for tooth grinding treatment in Melbourne or considering speaking with a qualified clinician, this guide will walk you through what to know, what to watch for, and when to seek personalised advice.
What is Bruxism?
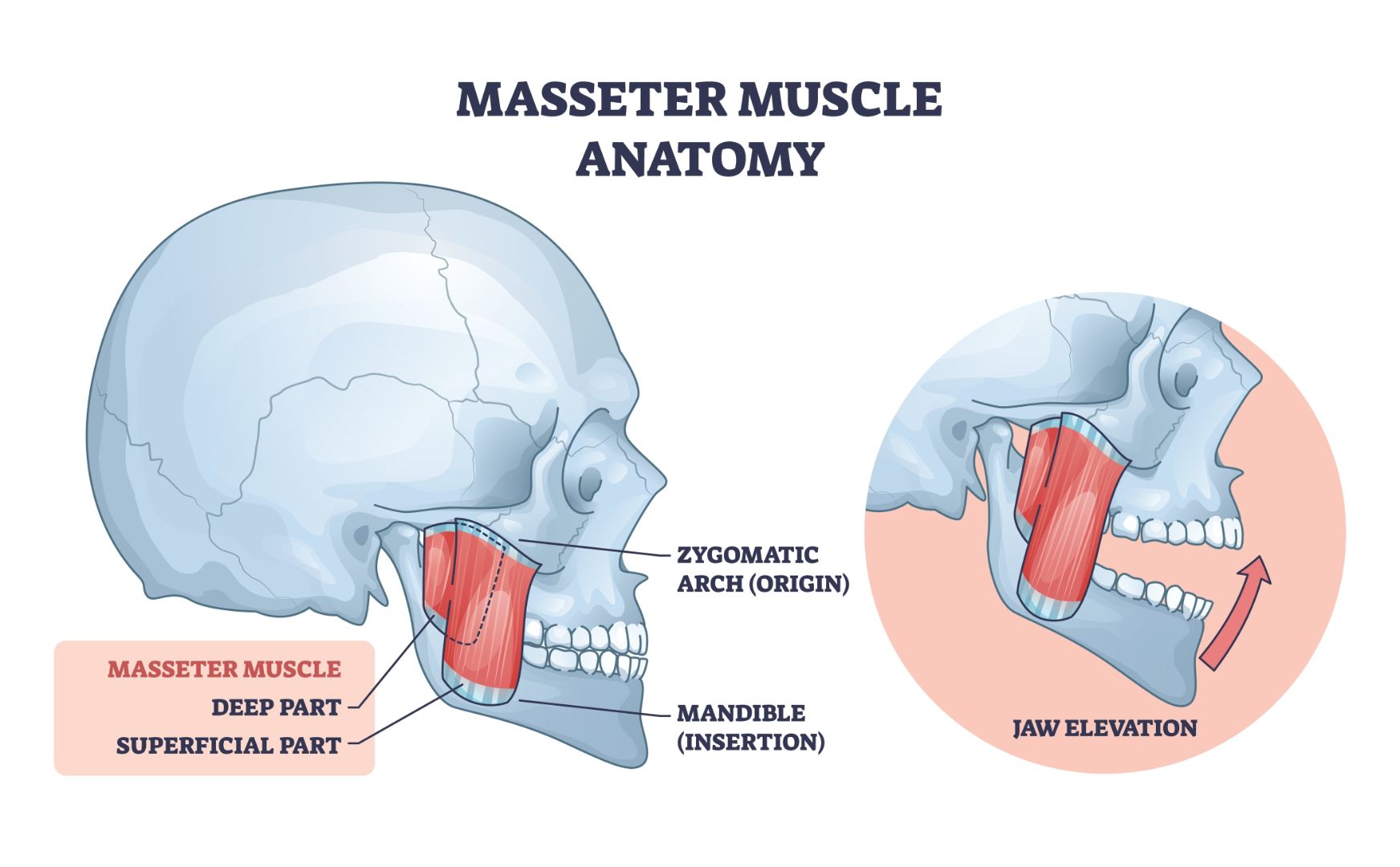
Bruxism refers to repetitive teeth grinding or jaw clenching, often occurring without conscious awareness. It can contribute to jaw tension, tooth wear, and disrupted sleep, making early recognition important for overall oral health.
Awake vs sleep bruxism
Awake bruxism typically presents as daytime jaw clenching, often linked to stress, concentration, or habitual behaviours like resting the teeth together. In contrast, sleep bruxism occurs involuntarily during sleep cycles and may be associated with sleep disturbances. Many people are unaware of sleep bruxism until symptoms such as morning jaw pain or partner-reported grinding sounds emerge.
What Causes Teeth Grinding?
Understanding the causes of teeth grinding is key to recognising why jaw clenching and bruxism symptoms develop. In many cases, there isn’t a single trigger, but rather a combination of lifestyle, biological, and behavioural factors that contribute to ongoing jaw tension.
Psychological factors: stress and anxiety
Stress is one of the most commonly reported contributors to bruxism. People experiencing high workloads, emotional pressure, or disrupted routines may unconsciously clench their jaw during the day or while asleep. This repeated tension can lead to jaw pain, tightness, and even morning headaches.
Sleep-related factors
Sleep bruxism is often linked to irregular sleep patterns or disturbances during the night. While not always noticeable, it can occur alongside fragmented sleep or brief arousals, which may contribute to ongoing teeth grinding and reduced sleep quality over time.
Lifestyle influences
Certain everyday habits can increase the likelihood of jaw clenching or grinding. These include:
- High caffeine intake, particularly later in the day
- Alcohol consumption, which may affect sleep cycles
- Some medications that influence muscle activity or sleep patterns
Dental and bite factors
In some individuals, the way the upper and lower teeth meet—known as occlusion—can play a role. Bite irregularities or existing tooth wear may contribute to grinding patterns, although they are rarely the sole cause.
Posture and habitual behaviours
Poor posture, particularly forward head positioning from prolonged screen use, can place strain on the jaw muscles. Combined with habits like gum chewing or resting the teeth together, this may reinforce patterns of jaw clenching and tension.
Signs and Symptoms to Look Out For
Recognising bruxism symptoms early can help you take practical steps before jaw tension or tooth wear progresses further. While experiences vary, there are several common patterns that may indicate ongoing teeth grinding or jaw clenching.
Pain-based symptoms
One of the most noticeable signs is waking with jaw pain or stiffness, often accompanied by morning headaches that sit around the temples. This discomfort can ease throughout the day but may return after periods of stress or concentration, reflecting ongoing jaw muscle overuse.
Dental indicators
Changes in your teeth can also point to bruxism. Gradual tooth wear, flattening of the enamel, or small chips may develop over time. Increased tooth sensitivity, particularly to hot or cold, can also occur as the protective enamel layer becomes compromised.
Joint-related symptoms
The temporomandibular joint (TMJ), which connects the jaw to the skull, may become affected by repeated clenching. Some people notice clicking, popping, or a feeling of tightness when opening and closing the mouth, which can overlap with TMJ symptoms.
Facial changes
Over time, persistent jaw clenching can influence the appearance of the lower face. The jawline may appear broader or more square due to increased muscle activity, which is sometimes linked to masseter hypertrophy.
Sleep disruption
Sleep quality may also be affected, even if you’re not aware of the grinding itself. In some cases, a partner may notice grinding sounds at night, or you may wake feeling unrested despite a full night’s sleep.
Everyday Strategies That May Help
Stress and sleep management
Managing stress is often a key part of reducing jaw clenching. Techniques such as mindfulness, gentle exercise, or winding down before bed may support better sleep quality and could help to reduce the likelihood of sleep bruxism. Establishing a consistent sleep routine can also help minimise disrupted sleep patterns linked to grinding.
Jaw-awareness techniques
Becoming more aware of your jaw position throughout the day could make a meaningful difference. A commonly recommended approach is to keep the lips together while allowing the teeth to remain slightly apart, which may reduce unconscious clenching.
Physical relief strategies
Simple physical measures may help to ease jaw pain and muscle tightness. Applying a warm compress to the jaw area, staying well hydrated, and practising gentle jaw stretches may provide short-term relief from tension.
Habit modification
Reducing strain on the jaw is another important step. This may include:
- Limiting chewing gum and very tough foods
- Avoiding habits like nail biting or pen chewing
Dental support
If teeth grinding persists, speaking with a dentist about an occlusal splint may be beneficial. This type of appliance is designed to protect the teeth from wear and may help reduce strain on the jaw over time.
Wrinkle Treatments for Bruxism

In some cases, people exploring support for ongoing jaw tension may also discuss the role of wrinkle treatments with a qualified clinician. When used in the lower face, these treatments may be considered as part of a broader, individualised approach to managing muscle-related concerns such as clenching. The goal in this context is not cosmetic alone, but to assess how reducing excessive muscle activity might influence symptoms like jaw tightness or discomfort. It’s important to note that suitability varies from person to person, and any decision to proceed is made following a thorough consultation, where your clinician can explain potential considerations based on your anatomy and concerns.
When to Speak to a Qualified Clinician

Knowing when to seek professional advice for bruxism treatment could help prevent ongoing jaw pain, tooth wear, and long-term changes to the jawline. While mild jaw tension or occasional teeth grinding may settle with lifestyle adjustments, persistent or worsening symptoms should be assessed by a qualified clinician.
Key indicators for seeking help
There are several signs that suggest it may be time to move beyond self-management and explore professional guidance. These include:
- Ongoing jaw pain or tightness, particularly in the morning
- Frequent headaches linked to jaw tension
- Noticeable tooth wear, chipping, or sensitivity
- Clicking, popping, or discomfort in the TMJ
- Changes in facial shape, such as a broader jawline
If you’re experiencing one or more of these symptoms, a clinical assessment can help clarify what may be contributing to your bruxism symptoms.
What a consultation typically involves
A consultation is designed to build a clear understanding of your concerns and overall health. This usually includes a discussion of your symptoms, lifestyle factors such as stress or sleep quality, and a physical examination of the jaw, teeth, and surrounding muscles. Your clinician will then explain potential management pathways and discuss whether further assessment or tailored support may be appropriate for your individual needs. Bruxism is a common yet sometimes overlooked condition that can affect everything from sleep quality to jaw comfort and even facial appearance over time. Gaining a clear understanding of your symptoms is an important first step towards making informed decisions about your care.
If you’re noticing ongoing jaw tension, tooth wear, or changes in your jawline, speaking with a qualified clinician about bruxism treatment can help you explore what’s happening and what options may be appropriate for you. At Cityskin, we can provide a personalised consultation to discuss your concerns and guide you through suitable next steps in a supportive, professional setting.
Book a consultation to discuss your jaw tension with one of our qualified clinicians.
This article is general educational information and is not a substitute for personalised medical advice. Please speak with a qualified healthcare professional about your individual circumstances.
Frequently Asked Questions:
Bruxism is not always a permanent condition, and its intensity can vary over time. For some people, teeth grinding or jaw clenching may reduce as stress levels change or sleep improves. However, if underlying factors such as ongoing anxiety, sleep disruption, or habitual jaw tension remain, symptoms may persist and require professional assessment.
Bruxism and temporomandibular joint (TMJ) disorders are related but not the same. Bruxism refers to the behaviour of grinding or clenching, while TMJ disorder involves dysfunction or pain in the jaw joint itself. That said, the two can occur together and may share overlapping symptoms such as jaw pain or clicking.
The right professional can depend on your symptoms. Dentists often identify tooth wear and may assess bite-related factors, while a GP can help explore broader health or sleep concerns. A qualified cosmetic clinician may assess muscle-related jaw tension and discuss suitable management options as part of a comprehensive consultation.
A consultation typically begins with a discussion about your symptoms, lifestyle, and medical history. This is followed by an assessment of the jaw, teeth, and muscle activity. Based on this, your clinician will explain potential pathways and whether further evaluation or tailored support may be appropriate for your individual situation.